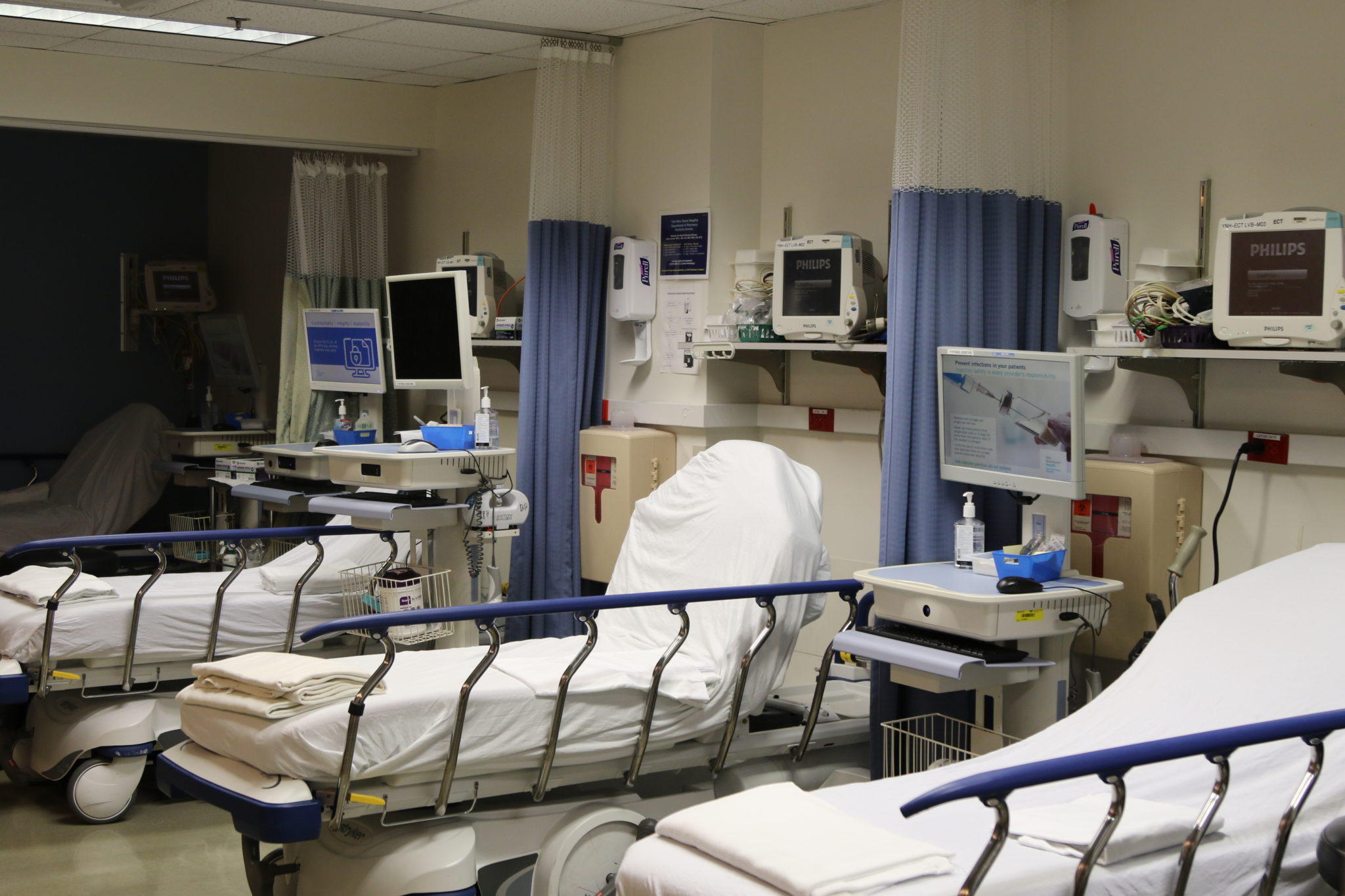
Marisa Peryer
The basement of the Yale New Haven Psychiatric Hospital where psychiatrist Brandon Kitay treats his patients is indistinguishable from any other clinical suite. It houses the same beds and privacy curtains and carries the same hints of antiseptic in the air. The only unique aspect of this nondescript room is a gray box and a set of silver metal electrodes.
“There are still physicians out in the community that will say — when I mention what I do for a living— they say, ‘You still do shock therapy?’” Kitay said.
“Shock therapy”is known to medical providers as electroconvulsive therapy, or ECT. The therapy evolved from a series of psychiatric treatments from the mid-to-early-20th century and is used today as a tool to reduce symptoms in treatment-resistant patients with depression. The goal of ECT, according to Kitay, is not to shock the patient, but rather to administer a quick pulse of electricity to the patient’s head in order to cause a therapeutic seizure.
Patients are first put under general anaesthesia and are then given a muscle-blocking medication that prevents convulsions during the seizure. Two metal electrodes are then placed onto the patient’s head. A mere secondslong shock — one with a voltage equivalent to that of a household electricity outlet — is administered. This shock disrupts brain activity and causes the patient to seize. According to Kitay, the entire procedure takes 10 minutes and is rather uneventful to watch.
“In terms of the numbers, I usually quote that [ECT is] about as safe, if not safer, than an outpatient colonoscopy — in terms of the adverse events that occur,” Kitay said.
Despite the therapy’s relative safety, ECT is not widely practiced by psychiatrists. State regulations often restrict its use, and providers must convince their patients that the stigma associated with the therapy — which is rooted in the treatment’s controversial past — does not reflect its current use.
When antidepressants fail
To Kitay, ECT is an underutilized tool to help patients who have not responded to antidepressants, one of the most common interventions used to treat patients with depression.
“Depressed patients that are started on a first-line antidepressant — only about a third of them will get better,” Kitay said.
Neither doctors nor patients will know whether a prescribed antidepressant will actually treat depressive symptoms until the medication reaches its full effect over the course of four to six weeks. Further treatment with different types of antidepressants may also prove ineffective.
“If we try another medication, only about another third will get better, which leaves a huge large swath — almost 30 percent of our patients — who will eventually meet criteria for clinically treatment-resistant,” he said.
Patients who qualify as treatment-resistant could go over a year without an adequate solution for their depression. Meanwhile, these patients must live with their symptoms, which can negatively impact relationships, school and work — the consequences of which may only compound their depression. But where antidepressants fail for treatment-resistant patients, ECT often succeeds, according to Kitay. And patients can see improvement as early as two weeks after their first treatment.
“The response rates for ECT reported in the literature are anywhere from 60 to 80 percent depending on the patient population that you look at — and that’s in a treatment-resistant population,” Kitay said.
Despite these impressive numbers, Connecticut has just five ECT centers, and some states like Nevada have only one. Government policy hampers patient access to the therapy for safety reasons. After being treated with ECT, patients may experience short-term memory loss, such as forgetting conversations or appointments. Some doctors have reported that patients have lost specific details from long-term memories.
“I have never encountered, nor is it common, for people to lose a large swath of their memory — their long-term memory, they forget who they are — that just does not happen with ECT,” Kitay said.
Impaired concentration and attention are core symptoms of depression, according to Kitay, who said that some of his patients have even reported that their short-term memory has actually improved with ECT.
According to University of Connecticut Health psychiatrists Srinath Gopinath and Eric Brueckner, who practice ECT, the government’s restrictive policy regarding ECT treatment also stems from the therapy’s unsavory past.
“There were a lot of issues with medical ethics during the time that ECT was being utilized; patients were given it in this barbaric way,” said Brueckner. “ECT’s history is not a pretty one, and so, for that reason, I think that the stigma is a big reason that it’s more difficult in certain states for patients to have access to ECT.”
During the 20th century, ECT was not performed in the same way that psychiatrists now administer the therapy. Back then, these procedures frequently took place in large mental institutions that were withdrawn from the public eye. Psychiatrists would experimentally administer treatment to their patients, who were often unable to give consent. And though ECT has evolved far past these practices, its history still stigmatizes the treatment today.
An approach in the midst of nihilism
A culture that accepted experimentally treating patients grew out of a crisis facing hospital psychiatry departments at the turn of the 20th century, said Deborah Doroshow GRD ’12, an oncologist and academic affiliate in the Yale School of Medicine’s section of the History of Medicine. The number of institutionalized patients soared, while the population of doctors staffing these hospitals failed to expand proportionally. Overworked and underfunded, Doroshow said that hospital psychiatrists were only able to dole out care to their patients — who presented a wide spectrum of disorders — in an custodial fashion with little individual attention.
Adding to the issue, medicine had yet to produce robust treatments for mental illness. Psychiatrists at the time were only able to placate, not treat, their patients, according to Andrew Scull, a psychiatry historian and professor of sociology and science studies at the University of California, San Diego.
“What happened in the early 20th century [is that] psychiatrists — who by then had fallen pretty far in most people’s estimations — decided, ‘Look, just being boarding house keepers, and keeping these people alive is not going to do much for our professional reputation,’” Scull said.
Beginning in the 1910s, psychiatrists began to experiment on their own patients, a trend enabled by the lack of legal safeguards given to the certified insane, according to Scull. The interventions developed during this period — including ECT — subjected the body to immense amounts of physical stress, in line with a popular theory at the time which proposed that treating the body could also treat the mind, Doroshow said.
When psychiatrists reported that their new treatments improved or cured their patient’s afflictions, the broader scientific community took note. Two Nobel Prizes for Physiology or Medicine were awarded to psychiatrists during this era of experimentation. Julius Wagner-Jauregg, an Austrian psychiatrist, won the first in 1927 for developing malaria therapy.
A 2013 report published in the Yale Journal of Biology and Medicine discussed the history of malaria therapy, a procedure that psychiatrists used to treat patients suffering from “general paresis of the insane,” which Scull said was caused by the third stage of syphilis. According to Scull, patients who suffered from this disease, which caused symptoms like paralysis and psychosis, were deliberately infected with the parasite that causes malaria.
“Sometimes what happened is that there were whole colonies of malarial mosquitoes kept in hospitals and you would put a patient in a straitjacket in a room and have them bitten by the mosquitos,” Scull said. “Alternatively, if a patient had malaria you would withdraw some of the blood, which had the malaria parasites in it, and inject them into a patient you wanted to treat.”
The fever that resulted from the malaria infection would cause patients to “sweat out” their mental malady — the efficacy of which is controversial, according to Scull.
The second Nobel Prize was awarded to Portuguese scientist António Caetano de Abreu Freire Egas Moniz, who won half of the 1949 award for “discovering the therapeutic value of the leucotomy,” a psychiatric treatment that severed brain tissue.
The leucotomy was brought to the U.S. by physician Walter Freeman II, class of 1916, and neurosurgeon James Watts. Freeman modified Moniz’s technique and renamed it the lobotomy, according to a 2017 paper published in the Journal of Neurosurgery.
Scull said that the lobotomy was first performed using typical surgical practice to reach the brain by drilling into the skull. But when this method proved too time consuming and expensive, Freeman used a new protocol — the transorbital lobotomy — in which access to the brain was gained through the eye socket.
“[Freeman] took an ice pick and a hammer and he gave patients a couple of electroshocks so they were unconscious,” Scull said. “Then he took the ice pick, slid it underneath the eyelid — up against the bone behind the eye — banged it with the hammer, wiggled it about to sever brain tissue, then pulled it back out.”
Freeman, who would sometimes perform up to 20 to 30 lobotomies a day, would often not bother to sterilize the instrument, according to Scull.
Popular media like “One Flew Over the Cuckoo’s Nest” and “Shutter Island” have portrayed therapies from this time period as exercises of control and punishment by hospital psychiatrists. Though this portrayal is not entirely false, according to Doroshow, most doctors at the time genuinely believed that they were acting in the best interests of their patients’ well being by administering these treatments.
“Why did something we think is so crazy now — why was it a standard treatment for so many decades?” Doroshow said. “And it’s because people were desperate. It made doctors feel optimistic — it was a new approach in the midst of a lot of nihilism. And patients seemed to be changing for the better.”
Instead of labeling practices like those used by psychiatrists in the 20th century as inhumane, Doroshow said that it is sometimes more worthwhile for historians to understand their broader historical context. Hospital psychiatrists of that era, she said, did not have the right tools or sufficient knowledge to treat mental illness effectively.
“As an internal medicine doctor who treats cancer patients, I can also tell you that we don’t know why all of our treatments work, either,” Doroshow said. “So it’s really easy to point fingers at psychiatrists and say that there is missing data, but even in oncology —which is a very data driven field — there is so much we don’t know.”
“Not again, it’s deadly”
During the same period of experimentation that produced treatments like malaria therapy and the lobotomy, ECT evolved rapidly from a separate set of therapies. The first in this series was insulin coma therapy, an intervention used to treat schizophrenia, which psychiatrists then called dementia praecox.
“Perhaps putting people into comas using insulin could be used to cure mental illness,” Scull said, explaining the therapy’s logic. “There really wasn’t any theory behind that — it was a bizarre theory instead of a carefully developed one.”
Insulin was hailed as a miracle drug in the late 1920s, when doctors were first able to use the hormone to treat children with Type 1 diabetes, Doroshow said. Its effectiveness for treating diabetes led doctors to experiment with potential other uses for the hormone, which included treating schizophrenia starting in the 1930s. In this therapy, hospital psychiatrists would induce comas in patients by administering large doses of insulin. After a predetermined amount of time, those patients would then be brought back to consciousness with a dose of glucose.
Insulin coma therapy was a dangerous and delicate procedure, according to Doroshow, one which required the constant attentiveness of medical staff. If patients were left comatose for even slightly too long, the treatment could result in irreparable brain damage or even death.
Psychiatrists at the time did not agree on the therapeutic effects of the treatment, Scull said. Some argued that patients’ symptoms improved because of the coma. Others asserted that convulsions — which occurred in some comatose patients — made patients better.
Soon after, in 1934, as insulin coma therapy grew more popular, a new synthetic drug called metrazol came onto the scene, and its use quickly spread throughout psychiatry. Hospital psychiatrists would administer the drug to patients in order to induce violent — and supposedly therapeutic — seizures to treat schizophrenia.
“The logic behind that one was that, allegedly, it worked for schizophrenia because you couldn’t be schizophrenic and epileptic simultaneously,” Scull said, explaining the theory, which has since been proven untrue. “So if you artificially induced epilepsy, it would drive out the schizophrenia.”
Though the treatment’s apparent effectiveness made doctors optimistic, metrazol-induced seizures also caused severe side effects, according to Scull. The drug caused convulsions so violent that patients would often fracture their spines or hip sockets as they seized.
“The period between the injection [with metrozol] and the convulsion could last for two, three, five, 10 minutes,” Scull said. “During that time, as the inventor of this technique himself acknowledged, the patient felt as though he or she was about to die. Imagine for a moment you are somebody who is paranoid and a white-coated person injects you with something, and you immediately feel as though you are going to die. Then, after an uncertain amount of time — if you’re lucky, because otherwise that feeling persists — you convulse violently.”
These distressing side effects of the unreliable treatment led psychiatrists to search for more effective alternatives for inducing seizures. Two Italian researchers named Ugo Cerletti and Lucio Bini offered a solution, which they called electroconvulsive therapy.
A recount of Cerletti and Bini’s early experiments with ECT was published in the journal Convulsive Therapy in 1988. The two first tested ECT on dogs by passing electricity through their hearts in order to induce seizures, but about half of their animals died after the electricity disturbed their normal heart function. According to Scull, the duo’s methods changed after they learned that butchers frequently stunned pigs before slaughter by shocking their heads with electricity.
“Literally, it was a visit to the slaughterhouse that lead Cerletti and Bini to try ECT on humans,” Scull said. “They tried it on some animals first to make sure they didn’t die, and they didn’t. Then they picked up a vagrant at the Rome train station, and they tried it on him.”
The scene was tense, Scull said. The first shocks to the vagrant did nothing, so Celetti decided to increase the amount of electricity administered.
“The patient, supposedly in one version of the story, turned to them and said, ‘Not again, it’s deadly,’ at which point they readministered the treatment and he seized,” Scull said.
The vagrant lost consciousness and briefly stopped breathing. After he regained consciousness shortly thereafter, he conversed coherently for a time after the treatment. Soon after this trial, according to Scull, Cerletti and Bini published their findings. Psychiatry quickly grabbed hold of ECT — a faster, cheaper and more reliable replacement for therapies like metrazol-induced seizures or insulin coma therapies.
Until 1941, ECT caused the same violent convulsions that metrazol produced, until psychiatrists began to administer muscle relaxants to patients before they were treated with the electricity. These muscle relaxants affected all of the body’s muscles, including those that act on the heart and lungs. Back then, according to Scull, most mental hospitals could not afford life-support equipment, or additional personnel to safely administer this modified ECT technique — so many opted for the unmodified method, putting the patient at high risk for fractures and other injuries as they convulsed during the seizure.
“These days, the ongoing use of ECT is virtually always done in the modified form — not with patients who are going to convulse in the old-fashioned way,” Scull said.
Combating stigma
As psychiatrists experimented with other uses for ECT outside of treating schizophrenia, they found that the therapy was reasonably effective in treating depression.
“It turned out, despite initial positive claims about its effect [on schizophrenia], it didn’t treat schizophrenia successfully,” Scull said. “But it did seem to have an effect on depressed patients, and so its use gradually shifted over to the treatment of depression.”
ECT enjoyed steady popularity throughout the mid-20th century until the ‘60s and ‘70s, when several movies portrayed the therapy as a way to punish patients instead of treat them. An anti-psychiatry movement gained traction during the same time, and psychiatrists and psychologists began to critique their own field, according to Marco Ramos, Jr. GRD ’17 MED ’18, a Yale psychiatry resident who studied psychiatric history as part of a graduate program on history of science and medicine.
“[Anti-psychiatry] reframed electroconvulsive therapy less as a therapeutic tool and more as a tool of social control and something that was violent,” he said.
The resurgence of ECT didn’t come until the turn of the 20th century, when a new body of research showed that the therapy effectively reduced symptoms in treatment-resistant depression, Ramos said.
According to Doroshow, ECT is one of the most effective interventions for treatment-resistant depression. But depressed patients already experience stigma, and a highly stigmatized treatment option like ECT that seems “drastic and scary” may actually turn patients away.
“Patients who undergo ECT still face enormous stigma, and increasingly, patients who have undergone treatment with ECT have started raising awareness on how useful the treatment has been to them in a number of cases,” she said.
One such patient, Kitty Dukakis, wife of former Massachusetts governor Michael Dukakis, published a book on her experience with ECT as a treatment for her depression, and has since been an outspoken advocate of the therapy.
But dismantling the stigma surrounding the therapy is difficult to address if psychiatrists and other medical professionals are not “on the same page” with regards to administering the therapy, Kitay said. The Accreditation Council for Graduate Medical Education requires that all psychiatry residents understand the risks, side effects and benefits of the treatment –– but they are not required to become proficient at administering ECT.
“Nowhere in the language does it say that the [psychiatry] resident has to be competent in actually delivering, or doing the treatments,” Kitay said. “And this opens up huge discrepancies or heterogeneity in ECT training experiences throughout the country,”
According to the UConnn Health psychiatrists Gopinath and Brueckner, the UConn School of Medicine offers an ECT elective for its psychiatry residents. They added that the medical school hopes to soon expand their ECT training.
Kitay said that some medical schools only require their psychiatry residents to attend a single hourlong lecture on ECT. But at Yale, all psychiatry residents are trained in the technique for four days at the clinic. Yale’s medical students are also required to attend lectures on ECT and to observe the therapy. A swath of medical professionals, including psychiatric nurse practitioners, nurses, social workers and pharmacists are even allowed to observe the treatments, according to Kitay, which allows them to better understand potential treatments their patients may receive.
“[Yale wants] ECT to be a less stigmatized, safe, outpatient therapy that people can access because they need it, Kitay said. “There aren’t many places like this.”
Marisa Peryer |marisa.peryer@yale.edu .







