Equity versus efficiency: Skirting state guidelines, Yale vaccinates all medical students regardless of patient contact
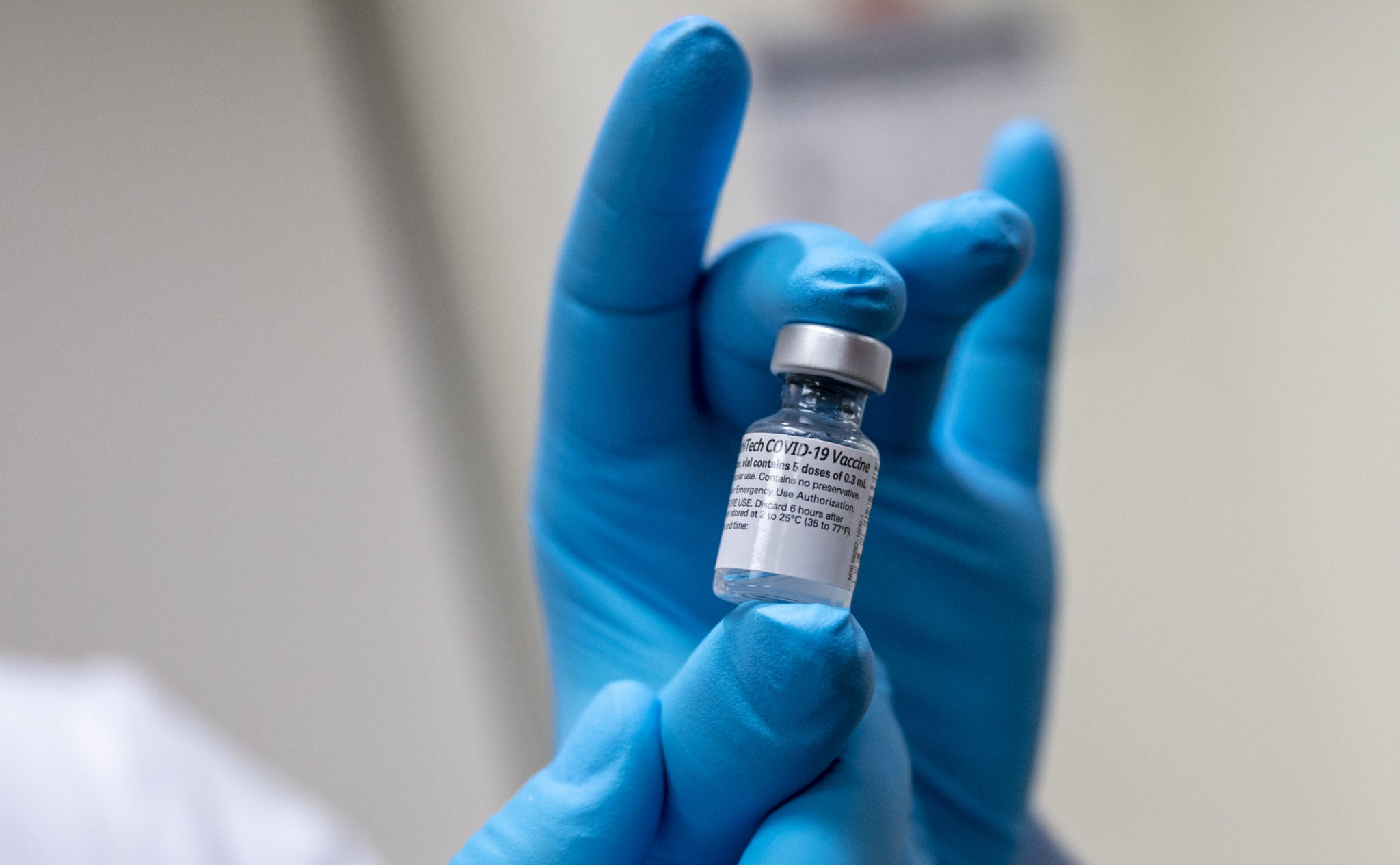
Wikimedia Commons
The University is using vaccines allocated by the state of Connecticut to immunize all medical students, even those removed from patient contact, in Phase 1a of the state’s vaccine rollout plan. The decision — which counters the spirit of state guidelines — has raised questions about whether it is equitable to prioritize non-patient-facing members of the population in vaccine rollout at elite, well-resourced institutions.
Maura Fitzgerald, spokesperson for the Connecticut Department of Public Health, said that the state only intended to include medical students in clinical rotations in Phase 1a. Yale, however, chose to offer vaccine appointments to all medical students.
University officials justified their allocation on the grounds that that all medical students could come into contact with patients. Additionally, it is difficult to determine which students might see patients, they said.
“I think there’s a very important balance between equity and efficiency here,” said Howard Forman, a professor at the School of Management and the School of Public Health. Vaccines should go to the most vulnerable and under-resourced communities first, but the perfect cannot be the enemy of the good, he said. Forman explained further that if there are extra vaccines left over — vaccines come in five- or ten-dose vials that must be used within hours — that might go to waste, they should go to someone even if they are not part of the primary group.
Some students expressed surprise at the plan, saying that a large portion of them do not interact with patients. Others said that the “arbitrary” vaccination plan happened quickly enough for the order not to make a significant difference in COVID-19 immunity.
Per Connecticut guidelines, the first round of vaccines was fast tracked to health care personnel, which the state defined as people serving in health care settings with the potential for direct or indirect exposure to patients or infectious materials. Still, Yale Health, which gets a supply of vaccines specifically earmarked for members of the Yale community, has distributed vaccines to students who do not come into contact with patients, according to a Jan. 4 email sent to those students.
“Please do not exclude yourself from this group even if you are not at this moment caring for patients,” the email reads. “If you exclude yourself from this group, you will lose all prioritization.”
The University decided to allow medical, physician assistant and nursing students to sign up for vaccines in reverse alphabetical order, regardless of whether they came into contact with patients. All of them have been invited to receive the vaccine over the next eight or nine weeks, according to Chief Executive Officer of Yale Health Paul Genecin.
That email contradicts what School of Medicine Dean Nancy Brown later told the News in a Jan. 24 email: that Yale Health is offering vaccinations to clinicians, medical students and physician assistants who interact with patients; researchers who are studying COVID-19; and clinical laboratory staff who work with samples that may contain live virus.
Genecin wrote to the News that vaccinating medical students in reverse alphabetical order was a way to randomize the invitation process and avoid privileging anyone. The University used the same approach to vaccinate health care workers at Yale Health, he added.
Genecin explained in a late January email to the News that all medical students are exposed to patients as soon as they start school, and that who comes into contact with patients can change rapidly. The best way to protect the students was to vaccinate them all, he said.
But in an interview with the News, Sumun Khetpal MED ’21 explained that medical students complete one and a half years of pre-clinical requirements before entering the hospital wards. It is not until the end of their second year and throughout their third year that students rotate through Yale New Haven Hospital and try out different specialties, Khetpal added.
Since receiving their vaccinations, some first-year medical students started having possible contact with patients this week. In the Interprofessional Longitudinal Clinical Experience courses, which were remote in the fall semester and at the beginning of the spring semester, faculty guide students on how to function in a clinical environment.
Fitzgerald, who is handling COVID-19 communications at the Connecticut Department of Public Health, said that the state’s intention with Phase 1a was to include only medical students in clinical rotations — not those in other stages of their education.
Department Chair of Epidemiology at the Yale School of Public Health Albert Ko said that because vaccines are a limited resource, particularly at the beginning of rollout, the chief public health priority should be to get the vaccine to people who have the highest risk of complications from the disease or of transmitting the virus to others. Ko told the News that health care workers and patient-facing medical students are included in that group.
“We really want this vaccine to go to our nursing home residents, to over seventy-fives, our health care workers,” Ko said. “The integrity of that program is going to be really key for this to be a public health success.”
But Associate Professor of Epidemiology Luke Davis noted that universities have to balance issues of equity with logistics. It is challenging, and potentially not feasible, to determine exactly which medical students might come into contact with patients, he said. Additionally, some students may not currently be seeing patients, but would maybe see them in the coming weeks or months.
The decision to vaccinate all medical students regardless of their level of current patient interaction was not the only point of complaint by students. Also puzzling to them was the decision to vaccinate those students in reverse alphabetical order by last name.
When she heard that all medical students would receive the vaccine, even if they are not patient facing, Aminah Sallam MED ’21 was surprised, she said. Yale was still vaccinating residents and fellows when medical students heard they would be getting the shot, too.
“Because they’re doing reverse alphabetical order of all health professional students, there’s a huge portion of those health professional students who, by the nature of the curriculum, do not interact with patients,” Sallam said.
Sallam had been going into the hospital throughout the pandemic, but she was not concerned about catching COVID-19. Because she does surgical rotations, patients she interacts with must have a negative COVID-19 test before their operations.
“That kind of was a source of frustration among students in terms of how arbitrary it felt,” Sallam said. “So you could have a student with a last name that began with A who would be at the end of the line but who would be in the middle of their clinical rotations get their vaccine after a first-year student who never comes into the wards and has a last name that begins with Z or Y.”
But Jonathan Avery MED ’21, who is doing rotations at the hospital this semester, said that though in theory the rollout would have disadvantaged him — due to his last name beginning with “A” — in practice, he was still quickly vaccinated. He added that he does not think he would have had any reasonable immunity earlier if students in the ICUs and emergency departments had been vaccinated first.
Still, Connecticut as a whole has been strapped for vaccine doses — last week, two hospitals in the state had to cancel vaccine appointments due to short supply. According to Connecticut Gov. Ned Lamont, 45 percent of the state’s population aged 75 and over has received their first dose of the vaccine.
Sydney Gray contributed reporting.
Rose Horowitch | rose.horowitch@yale.edu
Correction, Feb. 4: A previous version of this story implied that no first-year medical students come into contact with patients. It has been updated to include that starting this week, some first-year medical students will interact with patients, as part of the Interprofessional Longitudinal Clinical Experience courses.