Continuum of Care, a local organization that provides residential and support services to individuals with psychiatric or developmental disabilities, has launched the yearlong pilot of its Peer Connector program with the support of the Yale School of Medicine.
The medical school hosted its 23rd annual Hunger and Homelessness Auction last November to provide funding for six different local nonprofit organizations, including Integrated Refugee and Immigrant Services and Continuum of Care. Continuum is dedicated to working with the portion of the homeless population that has lost housing stability due to mental illness and substance abuse. This new project draws resources from Continuum’s South Central Peer Services division and its New Haven Crisis Stabilization program. It also incorporates a peer support system with its temporary housing services. Three months after the pilot’s launch, the program has one recovery support specialist working with five clients for 20 hours a week to ensure their mental and physical wellbeing after moving out of temporary housing and into their permanent communities.
“The peers, or we call them recovery support specialists, should be looked at like a point person who bridges the [clients from temporary housing] to their next placement,” said John Labieniec, clinical director of acute and forensic services at Continuum. “It makes discharge smoother when people feel comfortable with who they are working with.”
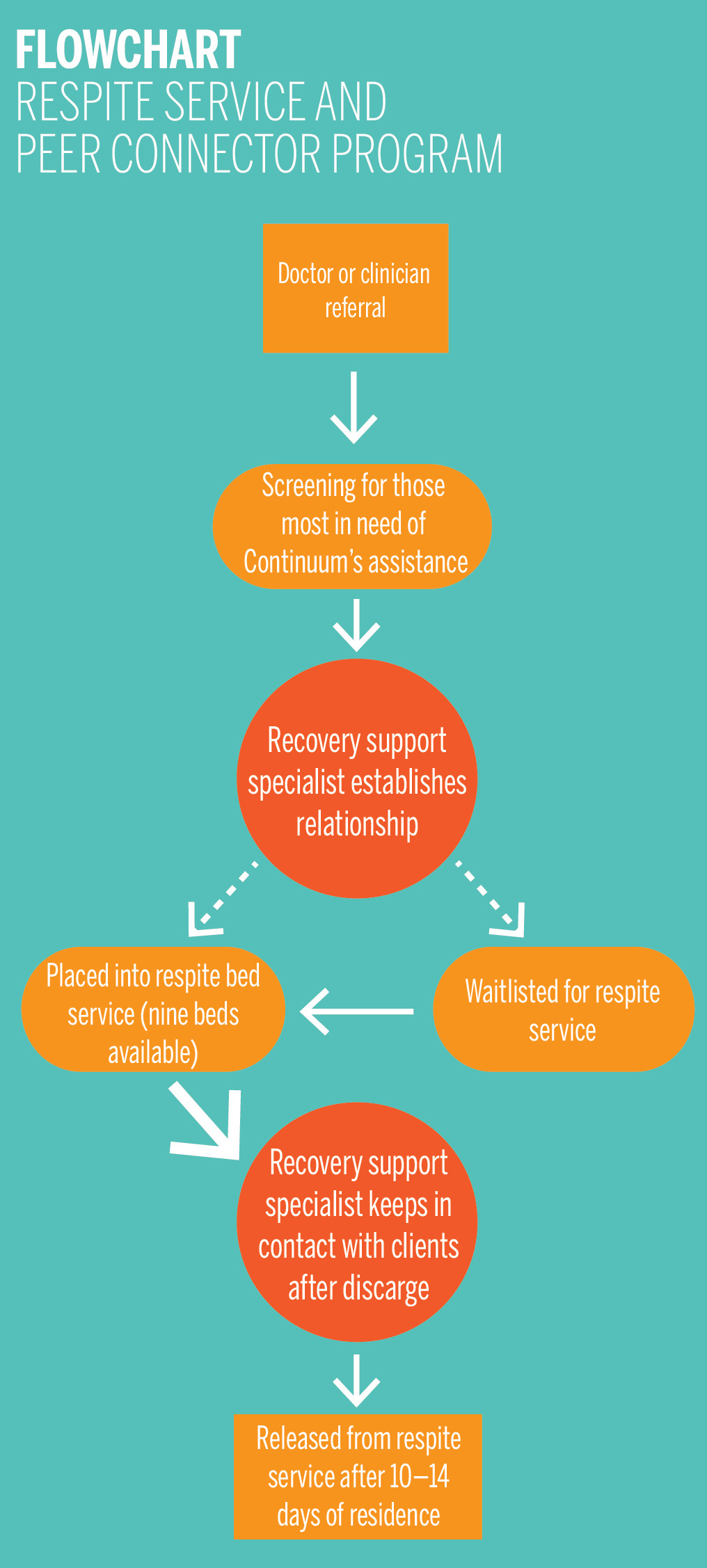
According to Labieniec, Continuum accepts patient referrals from emergency rooms, psychiatric hospitals and community members. The organization currently has nine beds allocated to the respite service in New Haven. However, the program receives 20 to 30 referrals a week, which is far more people than it can accommodate. As a result, the program’s managing team conducts screenings to select those they deem to be most in need of immediate attention. Usually referrals from emergency rooms are prioritized to avoid unnecessary hospitalization, Labieniec said.
Those selected from screening are either directly placed into one of the nine respite beds or on put on the waitlist. The program aims to create a home-like environment where clients can receive emotional and psychosocial support, Labieniec said.
“Many folks that we provide services to may have a difficult time in the shelter because of the level of stimulation that often comes with being in a shelter environment,” he said.
During the screening process, the team chooses a certain portion of the cases to assign to an individual called the “peer connector,” who must have a personal history of mental illness and homelessness. The peer connector is responsible for initiating long-term relationships that start before and end after the client uses the temporary housing service. Peer connectors are expected to contact clients before they arrive at respite and remain in touch after discharge to support clients through their treatment plans, SCPS Assistant Program Director Elsa Ward said.
“She’s the one that should say, ‘Hey, come on, if I could do it, you could do it,’” Ward said.
Aside from financial assistance for local housing and homelessness projects, the medical school also has a keen interest in evaluating the efficacy of the peer support system, said Chyrell Bellamy, psychiatry professor and a member of the Yale Program for Recovery and Community Health. Bellamy said she and her colleagues have been studying and initiating peer work for several years.
According to Bellamy, all the recovery support specialists must go through an 80-hour curriculum and pass a series of exam to be certified as a peer. She said she hopes as the profession advances, peer staff would be able to receive more equitable pay.
“The whole idea of peer support has just existed throughout life,” Bellamy said. “But in terms of it having a place within these formal settings, like in a hospital and a clinical setting, that’s fairly new.”
The Peer Connector program runs a budget of $19,050, more than half of which was granted by the medical school.







